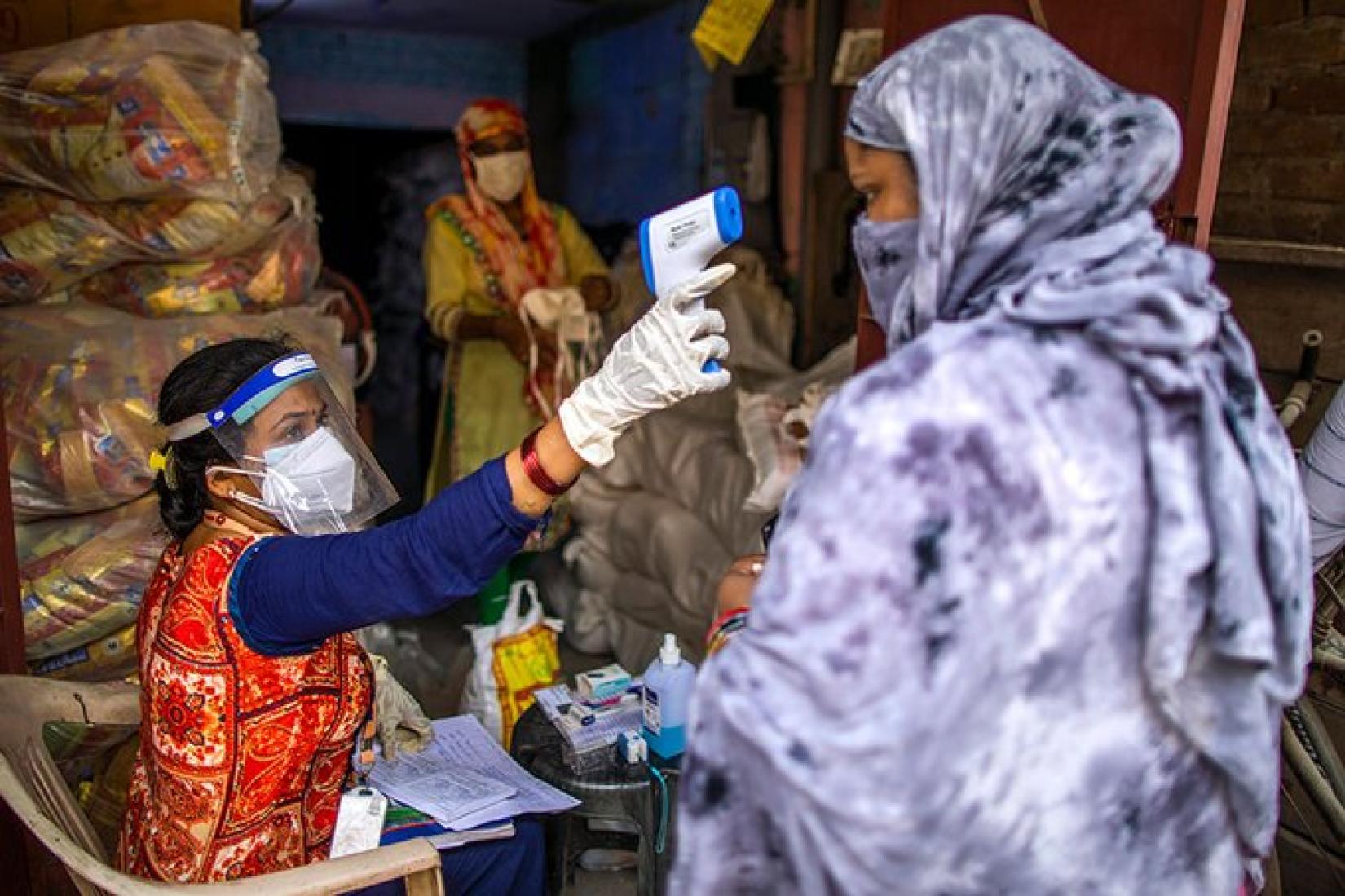
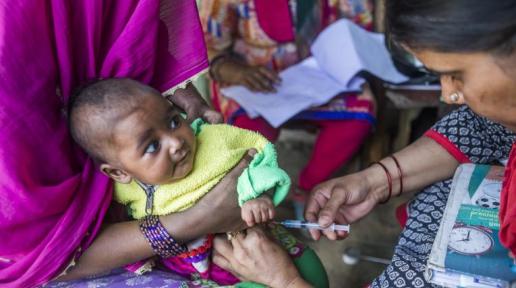
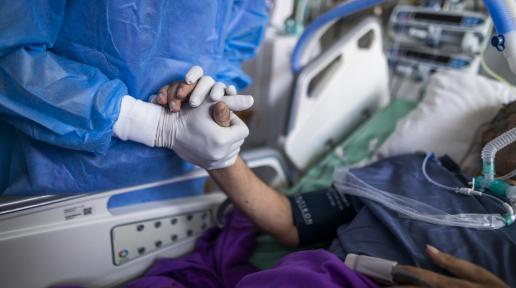
India has made considerable gains in health in the past two decades. Life expectancy at birth has risen from 63 years in 2000, to 70 years in 2019. By 2020, the infant mortality rate was 27 per 1,000 livebirths nearly 2.5 times lesser than in 2000. From 1990 to 2020, the newborn mortality rate (NMR) dropped by over half to 20 deaths per 1,000 livebirths, and the under-five mortality rate (U5MR) fell by nearly 75 percent to 32 deaths per 1,000 livebirths. Between 2000 and 2017, the maternal mortality rate (MMR) fell from 370 to 145 deaths per 100,000 livebirths.
The WHO declared India officially free from polio in 2014 and from maternal and neonatal tetanus in 2015. Family planning services and contraceptive prevalence has improved in most states. The incidence, prevalence and death rates from HIV/AIDS have also declined sharply in recent years. Similarly, there have also been significant reductions in the incidence of neglected tropical diseases and vector-borne diseases and shrinking of endemic areas.
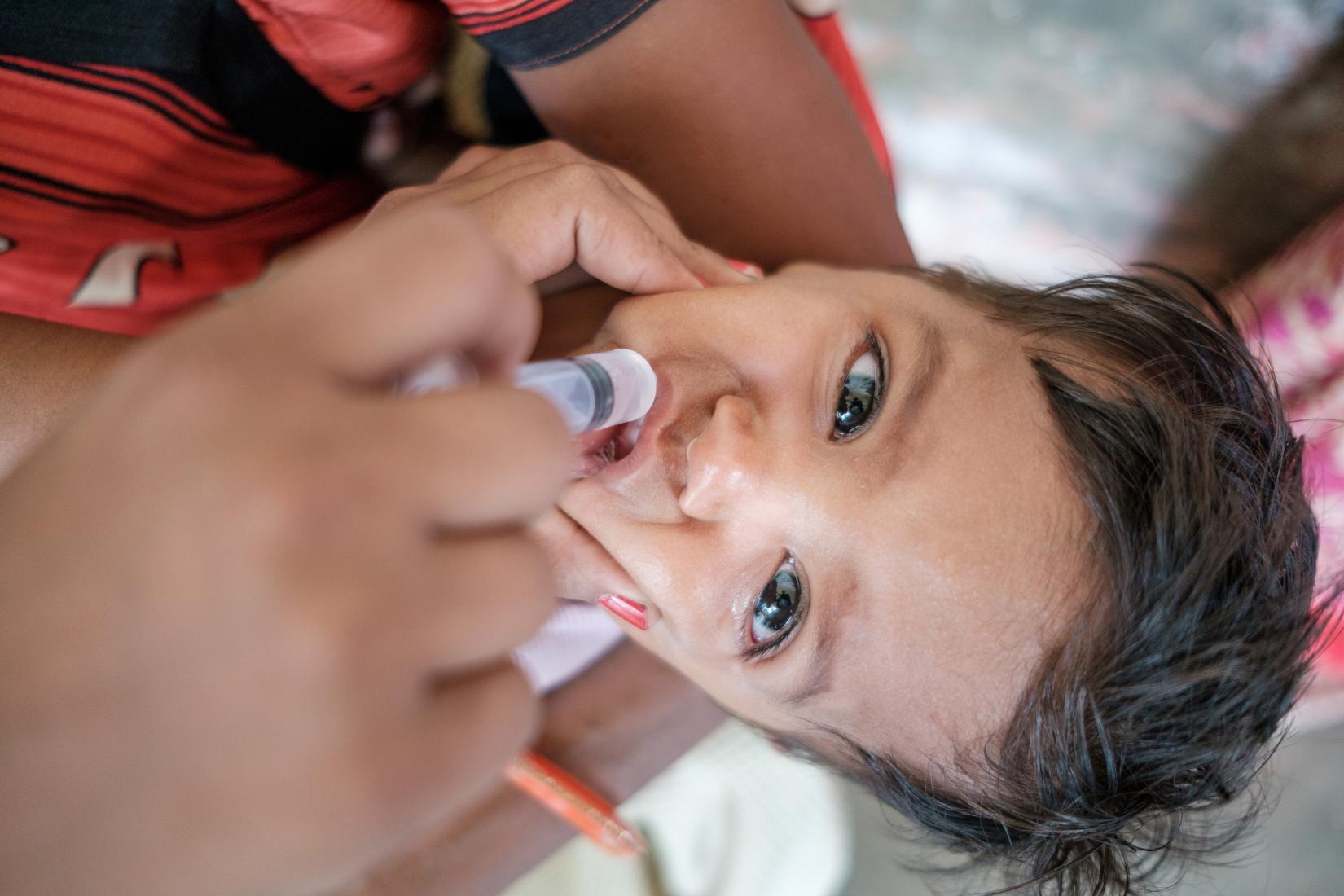
Challenges
In spite of the public health gains, the quality of maternal health services remains a major concern. With a stillbirth rate of 5 % (NFHS 4), India bears the burden of having the highest number of stillbirths globally; nearly 0.34 million of the 1.9 million stillbirths globally, happened in India in 2019. Moreover, nearly 35000 women continue to die due to pregnancy related complications which are largely preventable.
There is limited access to reproductive health services, especially among people living in interior rural areas and among marginalised young people. Access to sexual and reproductive health services is particularly limited among adolescents and young people.
India faces a high burden of both communicable and non-communicable diseases. Tuberculosis, lower respiratory infections, diarrheal diseases, malaria, and typhoid continue to be leading causes of communicable illness. There is a major upsurge in neglected tropical diseases including dengue and chikungunya, while kala azar, visceral leishmaniasis and leprosy continue to pose major health challenges, particularly in certain geographical areas.
Emerging and re-emerging disease such as H1N1 flu virus, SARS, Ebola and Zika pose a major health security threat, as do natural and man-made emergencies. Prevalence of cardiovascular diseases and diabetes are also a cause of concern.
Despite the headway made in the last two decades, several challenges remain. The government’s health expenditure has remained at around 1% of GDP over the past decade, which puts India significantly behind than the global average. These funds are also not efficiently utilised due to fragmented planning and vertical disease programmes.
The Economic Survey 2020-21 has strongly recommended an increase in public spending on healthcare services from 1 percent to 2.5-3 percent of GDP, as envisaged in the National Health Policy 2017. It notes that this can significantly reduce the Out-of-Pocket-Expenditure (OOPE) from 65 per cent to 35 per cent of the overall healthcare spend.
The private sector, which provides care to about 70% of the population, is unregulated and poorly integrated into health service delivery systems, despite the lack of infrastructure and human resources in the public sector. Access to life-saving drugs remains a challenge despite India’s role as a global pharmacy.

The Ministry of Health and Family Welfare recognises additional health challenges including: occupational health needs in both the formal and informal sectors, neglect of adolescent health, steady rise in mental illnesses, increased requirement of geriatric care, declining child sex ratios as well as the need to address the social determinants of health in the context of rapid economic growth and changing life styles.
COVID-19
572 million confirmed cases and over 6 million deaths worldwide, COVID-19 has changed the world as we knew it. The pandemic has enormously challenged health facilities and workers in India and across the globe.
India confirmed its first case of COVID-19 in February 2020 and has been grappling with the devastating health and socio-economic fallout of the pandemic ever since. 43 million cases and more than 0.5 million deaths later, India has been amongst the most impacted countries. The disease has exposed the gaps in public health infrastructure which could be attributed to long-term underspending on health.
The United Nations team in India worked across all 28 states and Union Territories, repurposed about half of its budget and approximately 80 percent of planned activities towards the COVID-19 response. Two strategic plans were developed by the UN in India to support the Government of India in its fight against the pandemic – Joint Health Response Plan and The Socio-Economic Response Framework.
For more details on UN India ‘s COVID response read the Annual Report 2020.

Water and Sanitation
India has made rapid progress in providing drinking water and safe sanitation to urban and rural households. As of June 2021, 43.5 million rural homes have been provided with piped water access.
Due to the success of Swachh Bharat Mission, which for the first time focused on outcomes (usage) and not outputs (toilets). Through the rural component of this mission (SBM-Grameen), India has achieved universal sanitation coverage in rural areas. It was estimated that the Universal Sanitation coverage has contributed in preventing 300,000 deaths over 5 years. Through phase 2 of SBM, efforts are now underway to ensure that open defecation free behaviours are sustained, no one is left behind, and that solid and liquid waste management facilities are accessible. Similar efforts are underway in urban areas through the Swachh Bharat Mission – Urban.

Swachh Bharat Mission Phase-II, launched in 2020 after 110 million households were provided with access to toilets during Phase I, focuses on the entire supply chain related to improving waste management, from faecal sludge to solid waste such as plastics.
The Government of India has also prioritised Jal Jeevan Mission (JJM) implementation, aiming to provide universal access to household tap connections in rural India by 2024.
Challenges
A critical challenge is to reduce the high microbial contamination of water sources, especially in rural areas. This is exacerbated by the lack of reliable data on water quality. It is estimated that around 37.7 million Indians are affected by waterborne diseases annually. In 2015, an estimated 117,000 under-5 children died of diarrhoea alone, representing 13 percent of all deaths amongst under-5 children, and 22 percent of the global burden. An estimated 73 million working days are lost due to waterborne disease each year, and the economic cost is estimated at US $600 million a year.
India has only 4 percent of the global water resources against 18 percent of the global population. The annual utilizable water resources in the country are 447 BCM from groundwater and 690 BCM from surface water Over 80% of the rural and urban domestic water supplies in India are served by groundwater. 255 Districts and 1,597 Blocks across the country has been identified as water stressed, by the Ministry of Jal Shakti (MoJS). As per the Central Ground Water Board, almost the whole country showed decline in water level in 2017, maximum fall was observed in and around parts of Rajasthan, Haryana, Punjab, Gujarat, Telangana, and Maharashtra.
Significant gaps exist in wastewater treatment across various states, with little improvements in the last three years, according to NITI Aayog’s Composite Water Management Index (2019), which enables monitoring of actions taken by states for effective water conservation and management. With only 31% of the industrial and domestic sewage (generated from 23 big cities) being treated and the rest being disposed as raw sewage into the water body is making water pollution a major concern for India.
Government initiatives
The Government of India has demonstrated its commitment to the overall well-being of its citizens. Back in 2005, the central government established the National Health Mission and introduced structural reforms to strengthen health care and sanitation. The National Health Policy 2017 clearly articulates the government’s commitment to reforming the health sector and achieving universal health coverage, not least by proposing an increase in the health budget to 2.5% of GDP. The policy also sets bound targets for disease elimination, reduction of premature and preventable mortality, systems strengthening, as well as improving health services. The government launched Mission Indradhanush in 2015 to rapidly increase immunisation coverage. It is also investing significant resources towards ending open defecation by 2019 through the Swachh Bharat programme.
UN's support
Towards Universal Health Coverage
- The UN in India will support the implementation of the National Health Policy and the Ayushman Bharat - National Health Protection Scheme, and its priorities for achieving Universal Health Coverage and Government’s on-going efforts to promote universal access to health, water and sanitation with the following expected results:
- Accelerate UHC and strengthen the health system’s capacity to provide quality health services for all, with a focus on reducing the financial burden on poor and marginalised groups
- Complete the un-finished MDG Health agenda, including universal access to voluntary and rights-based HIV care and treatment, sexual and reproductive healthcare and family planning services, especially for adolescents and young people
- End epidemics of key communicable diseases, including HIV, TB and hepatitis, and reduce maternal and new-born deaths
- Respond to the emerging challenges of non-communicable disease and environmental hazards
- Strengthen capacity to implement International Health Regulations to tackle health security threats from emerging and re-emerging diseases as well as disasters
- Step-up the response to the threat of antimicrobial resistance
- Eliminate neglected tropical diseases such as kalaazar leprosy and lymphatic filariasis
- Enhance national and state capacities to respond to drug abuse by strengthening prevention, treatment and care service.
Towards ODF free communities and water management
- Accelerate sanitation coverage leading to ODF communities
- Develop the capacity of stakeholders and communities, especially women, to undertake safety planning to mitigate the issue of water contamination
- Develop national capacity for integrated water resources management (IWRM) including surface water and groundwater resources.